You are in the middle of an ordinary day when your heart suddenly races. Your chest tightens. Breathing feels impossible. A wave of terror floods your body — and afterward, the fear of the next attack lingers.
Millions of U.S. adults live this cycle. According to the National Institute of Mental Health (NIMH), panic disorder affects approximately 2.7% of adults each year.
Short-term fixes — medication alone, reassurance seeking, or avoiding triggers — often reduce symptoms temporarily. But without skill-building, relapse rates remain high. Avoidance expands. Life shrinks.
For a broader foundation, see our guide on Signs of Mental Health Issue: The Ultimate Guide to Panic Attacks: Causes, Symptoms & How to Overcome Them for Good (2026)
What Is Long-Term Recovery From Panic Attacks?
A panic attack is a sudden surge of intense fear or discomfort that peaks within minutes and includes physical symptoms such as:
- Rapid heartbeat
- Sweating or trembling
- Shortness of breath
- Chest discomfort
- Dizziness
- Nausea
- Fear of losing control or dying
These symptoms result from activation of the body’s fight-or-flight response — even when no real danger exists.
Panic Attacks vs. Panic Disorder
A single panic attack does not equal panic disorder.
Panic disorder involves:
- Recurrent, unexpected panic attacks
- At least one month of persistent worry about future attacks
- Behavioral changes to avoid triggers
Many individuals experience isolated panic attacks without developing the disorder.
For a broader foundation, see our guide on Signs of Mental Health Issues: What Is Panic Attacks? A Complete Beginner’s Guide for Readers (2026)
What Long-Term Recovery Actually Means
Long-term recovery from panic attacks means:
- Minimal or zero attacks for 12+ months
- No life-limiting avoidance behaviors
- Ability to work, travel, socialize, and function without fear dictating choices
It does not mean never feeling anxious again.
It means anxiety no longer controls your decisions.
Why Many Definitions of “Recovery” Fail
Temporary symptom reduction is not true recovery.
Medication-only approaches can help stabilize symptoms, but without CBT skills and exposure work, stress often reactivates the cycle.
True recovery builds:
- Tolerance of body sensations
- Cognitive flexibility
- Behavioral courage
- Lifestyle resilience
Why Long-Term Recovery From Panic Attacks Matters
Untreated or poorly managed panic disorder carries real long-term consequences.
Research shows higher rates of:
- Major depressive disorder (up to 50% comorbidity)
- Emergency room visits
- Work absenteeism
- Social withdrawal
- Substance misuse
Health and Quality-of-Life Costs
Chronic avoidance narrows life:
- Declining career advancement
- Relationship strain
- Missed travel and social events
- Increased healthcare costs
Avoidance strengthens fear pathways neurologically. Exposure weakens them.
Real-World Benefits of Sustainable Recovery
When long-term recovery is achieved:
- Work performance improves
- Sleep stabilizes
- Relationships strengthen
- Health anxiety decreases
- Confidence returns
Take 60 seconds:
Write down one area of life panic still limits. Awareness is the first recovery step.
For a broader foundation, see our guide on Signs of Mental Health Issues: Emergency Resources for Panic Attacks Globally: Get Help Right Now
How Long Does Long-Term Recovery Take?
Recovery is not instant — and realistic expectations protect motivation.
Typical Recovery Phases
Weeks 1–4
Noticeable symptom reduction using grounding and breathing tools.
Months 2–6
Active CBT skill-building and structured exposure. Most see major improvement here.
Months 6–12+
Maintenance phase. Attacks become rare or absent.
Full sustained stability often occurs between 6 and 18 months of consistent practice.
Factors That Influence Speed of Recovery
Accelerators:
- Daily skill practice
- Strong support network
- Addressing sleep, caffeine, depression
- Early intervention
Slowers:
- Severe avoidance
- Long untreated duration
- Inconsistent exposure practice
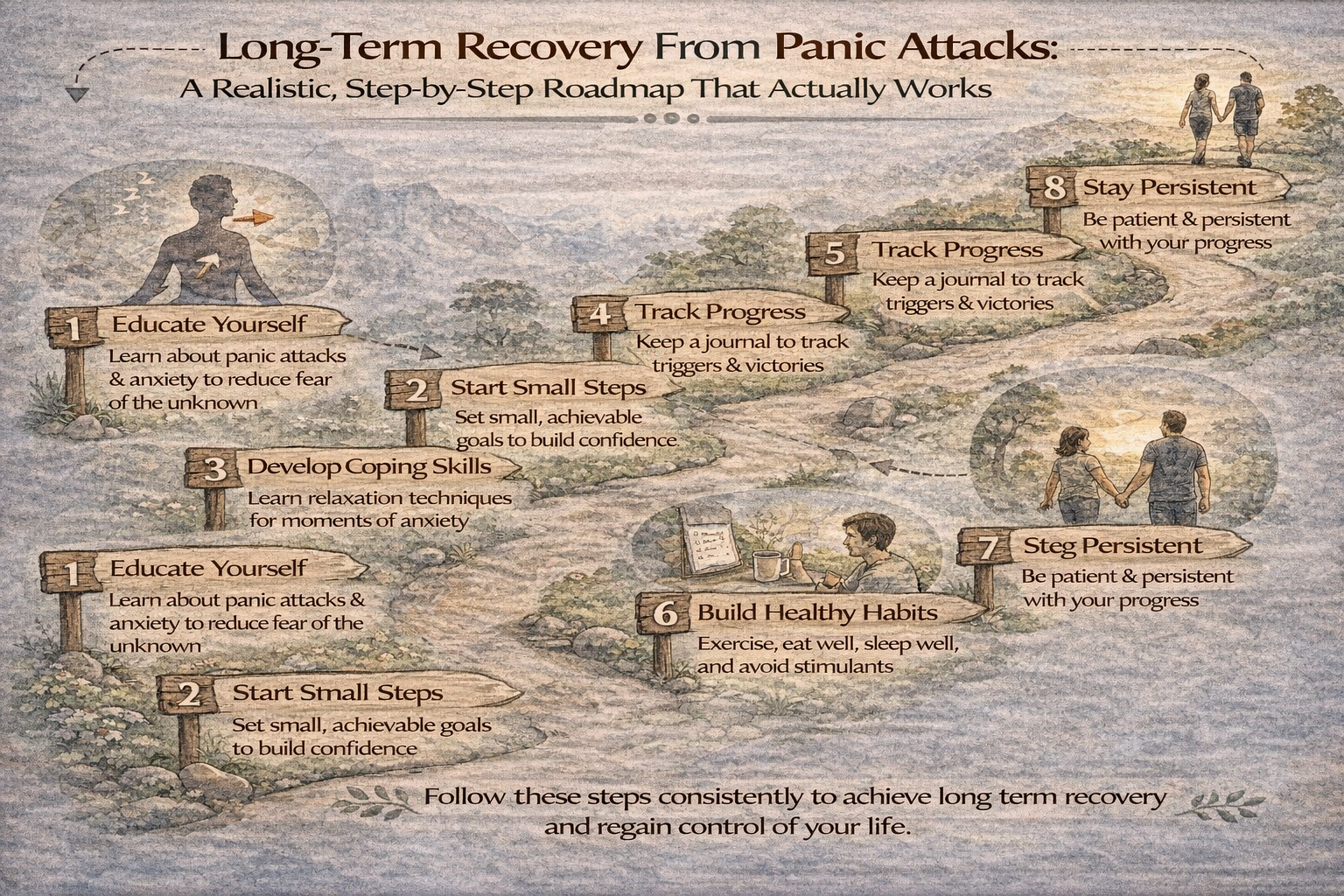
The Realistic Step-by-Step Roadmap for Long-Term Recovery
This section translates research into action.
Natural Methods That Support Nervous System Regulation
- Progressive Muscle Relaxation (PMR): 5–10 minutes daily
- Cold water exposure: activates the dive reflex
- Cardiovascular exercise: 30 minutes most days
- Consistent sleep schedule
Physical regulation lowers anxiety sensitivity — a core driver of panic disorder.
A Daily Routine That Builds Stability
Morning:
5-minute grounding (5-4-3-2-1 sensory exercise)
Midday:
Scheduled 15-minute “worry window”
Evening:
Screen-free wind-down 60 minutes before sleep
Structure reduces anticipatory anxiety.
Cognitive Behavioral Therapy (CBT) Skills at Home
CBT is considered first-line treatment by the Mayo Clinic.
Interoceptive Exposure
Intentionally recreate sensations safely:
- Run in place
- Spin in chair
- Breathe through straw
Goal: Teach the brain sensations are safe.
Thought Records
Write:
- Trigger
- Automatic thought
- Evidence for
- Evidence against
- Balanced thought
Behavioral Experiments
Test feared predictions gradually.
Medication-Free Recovery (When Appropriate)
Many individuals achieve remission without long-term medication.
If currently medicated:
- Never taper alone
- Work with a physician
- Build CBT skills before reducing dosage
Research shows CBT relapse rates (14–33%) are significantly lower than medication-only approaches in long-term follow-up.
Pro Tip:
Track attacks for two weeks: time, trigger, symptoms, response. Patterns reveal exposure targets.
Preventing Panic Attacks From Returning
Relapse prevention converts short-term success into lifelong stability.
Long-Term Management Plan
- Maintain exposure practice monthly
- Use 1–10 anxiety rating scale daily
- Quarterly “booster sessions” (self-review or therapist check-in)
4Identity Shift: Living Panic-Free
Move from:
“I am someone with panic disorder”
To:
“I am someone who knows how to manage anxiety.”
Celebrate weekly progress — small wins compound.
Scientific Evidence Supporting Long-Term Recovery
Structured CBT has strong longitudinal evidence.
- White et al. (2012): 67% remained in remission at 7-year follow-up
- Gloster et al. (2013): Gains maintained at 2 years
- Swoboda et al. (2003): 67% panic-free at 11-year follow-up
- Recent focused CBT trials show recovery rates above 70% compared to ~35% treatment-as-usual
A 2019 meta-analysis confirmed sustained benefits up to 12 months and beyond.
The National Institute of Mental Health continues to list CBT as a gold-standard intervention.
Common Mistakes in Long-Term Panic Recovery
Mistake 1: Expecting Overnight Results
Commit to 90 days minimum.
Mistake 2: Avoiding All Triggers
Avoidance strengthens fear circuits.
Mistake 3: Ignoring Lifestyle Foundations
Sleep, exercise, caffeine reduction are non-negotiable.
If experiencing suicidal thoughts, severe depression, or substance misuse, seek immediate professional care.
Frequently Asked Questions
What is the most effective long-term treatment?
CBT with exposure plus lifestyle stabilization shows the strongest evidence base.
How long until I feel normal again?
Most notice progress within 4–8 weeks. Stable recovery often forms between 6–12 months.
Can panic disorder fully go away?
Yes. Many individuals achieve full remission when skills are practiced consistently.
Is medication required?
Not always. Many recover without long-term medication under medical supervision.
Conclusion
Long-term recovery from panic attacks is not luck. It is a structured, repeatable process built on:
- Exposure
- Cognitive restructuring
- Nervous system regulation
- Lifestyle consistency
- Relapse prevention
This roadmap works because it targets root mechanisms — not just symptoms.
Start today:
- Identify one avoided situation
- Schedule one exposure step
- Practice one grounding skill
Sustained freedom is achievable. Research supports it. Clinical guidelines support it. Millions have done it.
Final Medical Disclaimer
This article is for educational purposes only and does not constitute medical advice. Always consult a licensed healthcare provider before making treatment changes. If in crisis, call 988 or visit the nearest emergency department.